Contact
Open Hours
Book an Appointment
Vaccines
Destinations
Pharmacy First
Access prescription medication directly from our pharmacist without seeing your GP for Ear infections, Impetigo, Infected insect bites, Shingles, Sinusitis and Throat Infections and UTIs in women
Repeat Prescriptions
Use our convenient online ordering service on your phone, tablet or pc. Get Reminders, Order 24/7, We keep you updated.
Pharmacy Services
We provide a full range of NHS and Private pharmacy services including one off and repeat prescriptions, private prescriptions and more.
Health Advice
Thousands of pages of health advice from the NHS, Pharmacists and Support groups covering every topic.
Blood Pressure Check
This service is a free NHS consultation from your Pharmacist, who will check your blood pressure and advise you on healthy lifestyle changes
Contraception Service
If you have a question about your contraception, need a repeat prescription of your pills or want to start on the pill for the first time, we offer the new Pharmacy Contraception service.
Our Best Services

Health Screening For Diseases
We provide Health Screening For Diseases

Vaccinations
Fever, headache, sore throat and all-over aches and pains are all symptoms that can be associated

Weight Management
A variety of weight management tools including Ozempic, Mounjaro and Wegovy to help you achieve your goals

Emergency Contraception
EHC is a method of contraception which may be used if a chosen form of contraception

Repeat NHS Prescriptions
Did you know that if you (or someone you care for) use the same medicines regularly you may not need...
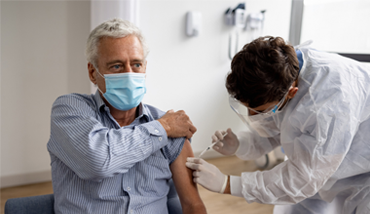
Private COVID-19 Vaccination Service
Protect Yourself and Your Loved Ones with Our Trusted Vaccination Service

Support for Care Homes
Support & Advice for Those in Care Homes & Special Care Homes

Stop Smoking
With the recent ban on smoking in public places. Many people are trying to quit smoking
View More Services
Kingsland Pharmacy
We are an independent NHS Community Pharmacy serving the people of London.
About
Kingsland Pharmacy
Welcome to Kingsland Pharmacy an NHS community pharmacy located at 406 Kingsland Road, Dalston, London, E84AA
Order Online
Order Online
On your Smartphone, Tablet or PC
Stores your items securely
Get reminders so you don't order your prescriptions too late
Order wherever you are 24/7
No need to get our engaged tone, we keep you updated
Chat to our Pharmacist
Get reminders so you don't order your prescriptions too late
Order wherever you are 24/7
No need to get our engaged tone, we keep you updated
Chat to our Pharmacist
Helping you to
Never Miss an Order
No more last minute panics! Set up prescription item re-order reminders so never get your items late again.
CONTACT
406 Kingsland Road
London
E8 4AA
London
E8 4AA
Email
02072546910
INFORMATION
Premises GPhC Number:
1091656
Superintendent:
Mukhtar Manji - 2035423
OPENING HOURS

